%201.svg)

Most people find out they snore from someone else. A partner's elbow in the ribs at 2 AM, a roommate's complaint, or waking up with a mysteriously sore throat — the snorer is usually the last to know.
That's because snoring is an airway problem, not a consciousness problem. During sleep, the muscles around your throat relax. If that relaxation narrows the airway enough, passing air causes the surrounding tissues to vibrate. That vibration is the sound you (or your unfortunate neighbor) hear.
Almost anyone can snore under the right conditions. A bad cold, too much alcohol, or an exhausting week can turn a non-snorer into a temporary snorer. The distinction that matters is where you fall on the spectrum: occasional snorer, chronic snorer, or someone whose snoring is a sign of something that needs medical attention.
According to the American Academy of Sleep Medicine, roughly 30% of adults snore regularly — and that number climbs with age.
Understanding what's behind your snoring is the first step toward fixing it. The causes generally fall into four buckets.
Some people are structurally more prone to snoring. A deviated nasal septum, enlarged tonsils or adenoids, a small or recessed jaw, or naturally narrow airways all reduce the space air has to move through. These aren't lifestyle choices — they're physical factors that make snoring more likely regardless of what you do before bed.
If you snore consistently and loudly even when you're not congested, not drinking, and not unusually tired, anatomy may be the primary driver.
Alcohol is one of the most direct snoring triggers. It relaxes throat muscles beyond their normal resting state, narrowing the airway further. Drinking within three hours of bedtime reliably worsens snoring for most people.
Excess body weight — particularly around the neck — compresses the airway from the outside. A neck circumference over 17 inches in men or 16 inches in women is associated with higher snoring risk. Smoking inflames airway tissues and reduces muscle tone, adding to the problem.
Sleep position matters too. Sleeping on your back allows your tongue and soft palate to fall backward, partially blocking the throat. It's one of the most controllable snoring triggers, and one of the easiest to address.
Building a consistent bedtime routine can help reduce many of these lifestyle triggers before they compound overnight.
Nasal congestion — from a cold, seasonal allergies, or dry air — forces mouth breathing, which bypasses the nose's natural airflow regulation and creates more turbulence in the throat. This type of snoring resolves once the congestion clears.
Extreme fatigue has a similar effect. When you're sleep-deprived, your muscles relax more deeply during sleep, making airway collapse more likely.
Men snore more than women — at least until midlife. Testosterone affects airway muscle tone and fat distribution around the neck. After menopause, however, women's snoring rates catch up considerably, likely due to hormonal shifts that affect muscle relaxation during sleep.

Not all snoring is equal. Simple snoring is a noise issue. Obstructive sleep apnea (OSA) is a medical condition — and the two can look identical from the outside.
OSA occurs when the airway doesn't just narrow but fully collapses, causing breathing to stop temporarily. These pauses (called apneas) can last 10–30 seconds and happen dozens or even hundreds of times a night. Each pause triggers a partial arousal that prevents deep, restorative sleep, even if you don't remember waking up.
The Sleep Foundation notes that untreated OSA is associated with elevated risk of high blood pressure, heart disease, and type 2 diabetes — making it a health issue that goes well beyond noise. Daytime impairment from sleep debt compounds over time when breathing disruptions go unaddressed.
STOP-BANG is a validated clinical screening tool used to estimate OSA risk. Score one point for each "yes":
A score of 0–2 indicates low risk. A score of 3–4 is intermediate. A score of 5 or higher puts you in the high-risk category and warrants a conversation with your doctor.
This tool is a screening aid, not a diagnosis. Only a sleep study (polysomnography) can confirm OSA.
See a healthcare provider if someone has witnessed you stop breathing during sleep, if you wake with morning headaches frequently, or if you're experiencing significant daytime sleepiness despite getting enough hours in bed. Loud, consistent snoring combined with any of these symptoms makes an evaluation worth scheduling.
The most effective snoring remedy depends on the cause. A one-size-fits-all approach rarely works — but working through these options systematically usually does.
Sleeping on your side is the fastest, cheapest fix for positional snoring. A body pillow can help you maintain the position through the night. Some people use the "tennis ball trick" — sewing a tennis ball to the back of a sleep shirt — to make back sleeping uncomfortable enough to avoid.
Elevating the head of your bed by 4 inches (not just stacking pillows, which can kink the neck) also reduces airway compression.
If nasal congestion is the primary cause, saline rinses before bed can clear the passage. Nasal strips (the external kind that physically widen the nostrils) help some people with nasal valve collapse but do nothing for throat-level obstruction. A humidifier in dry climates reduces tissue irritation.
Mouth tape — gentle tape applied over the lips to encourage nasal breathing — has become popular for mild snorers and mouth breathers. The evidence is limited but not harmful for most people (avoid if you have significant nasal obstruction).
Mandibular advancement devices (MADs) physically shift the lower jaw forward, opening the throat. For moderate snoring, these custom-fitted devices can be meaningfully effective. They're available over the counter in basic form or from a dentist for a fitted version.
For confirmed OSA, CPAP (continuous positive airway pressure) therapy remains the gold standard. It keeps the airway open with a gentle stream of pressurized air. Surgical options — such as uvulopalatopharyngoplasty (UPPP) or newer procedures like hypoglossal nerve stimulation — are typically considered when other approaches haven't worked.

One underappreciated challenge with snoring is feedback. You're asleep. You can't hear yourself. Unless someone else is tracking it, you have no idea whether the side-sleeping or the alcohol cut is actually making a difference.
That's where audio monitoring comes in. Alarmy's sleep analysis feature records overnight sounds and lets you listen back to what happened — powered by the app's RespireSegNet technology, which analyzes breathing patterns during sleep. Rather than guessing whether last night was better, you can actually hear it.
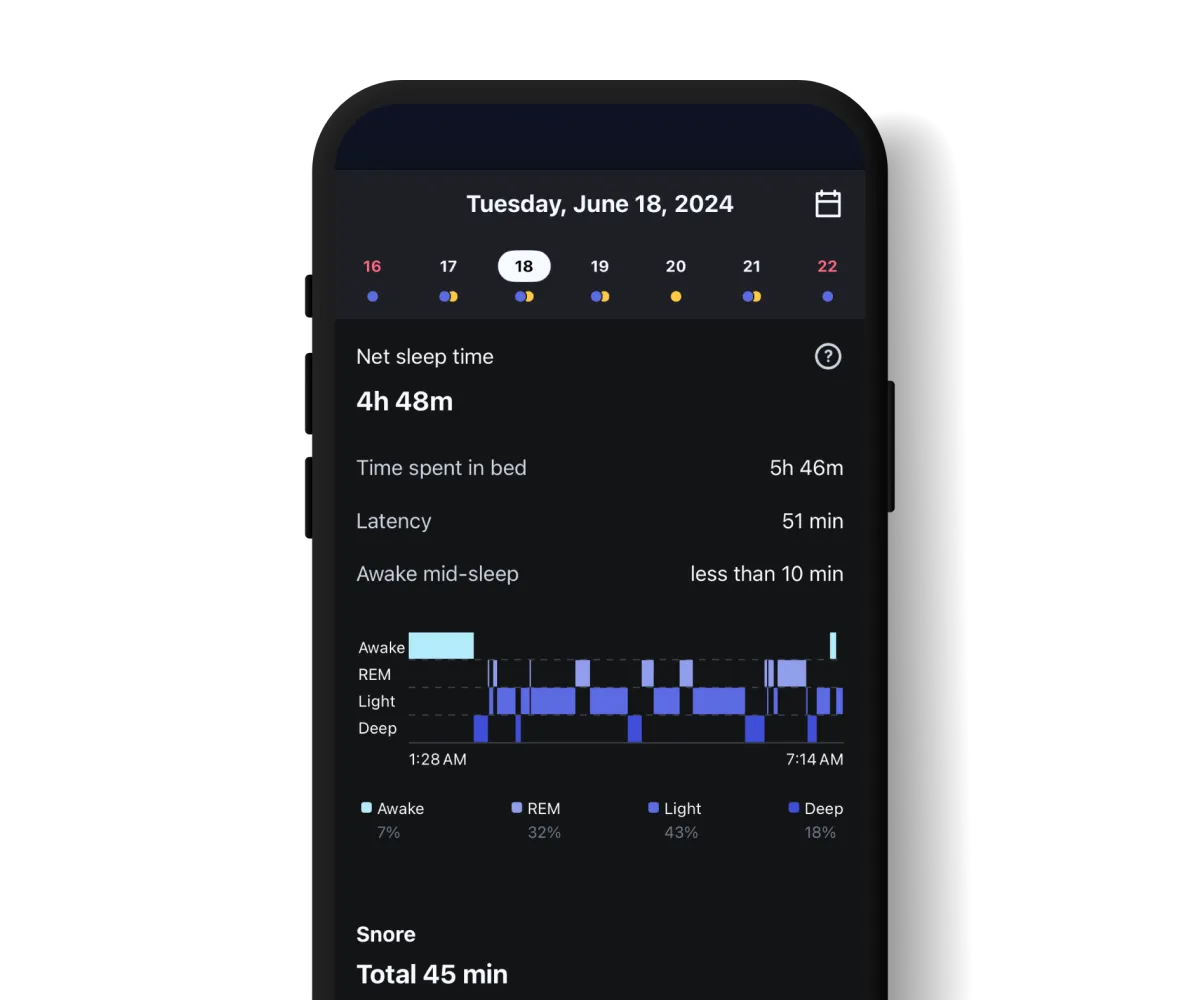
Use it as a baseline before you try any changes, then check again after two weeks of a new habit. The data won't replace a sleep study, but it gives you real signal instead of guesswork.
Snoring is common, manageable, and — in most cases — improveable. Start with the variables you control: sleep position, alcohol timing, nasal congestion. If symptoms point toward sleep apnea, get evaluated. It's a health issue worth taking seriously, not just a noise problem.
* This article is for informational purposes only and does not replace professional medical advice. Always consult a healthcare provider for health-related decisions.
